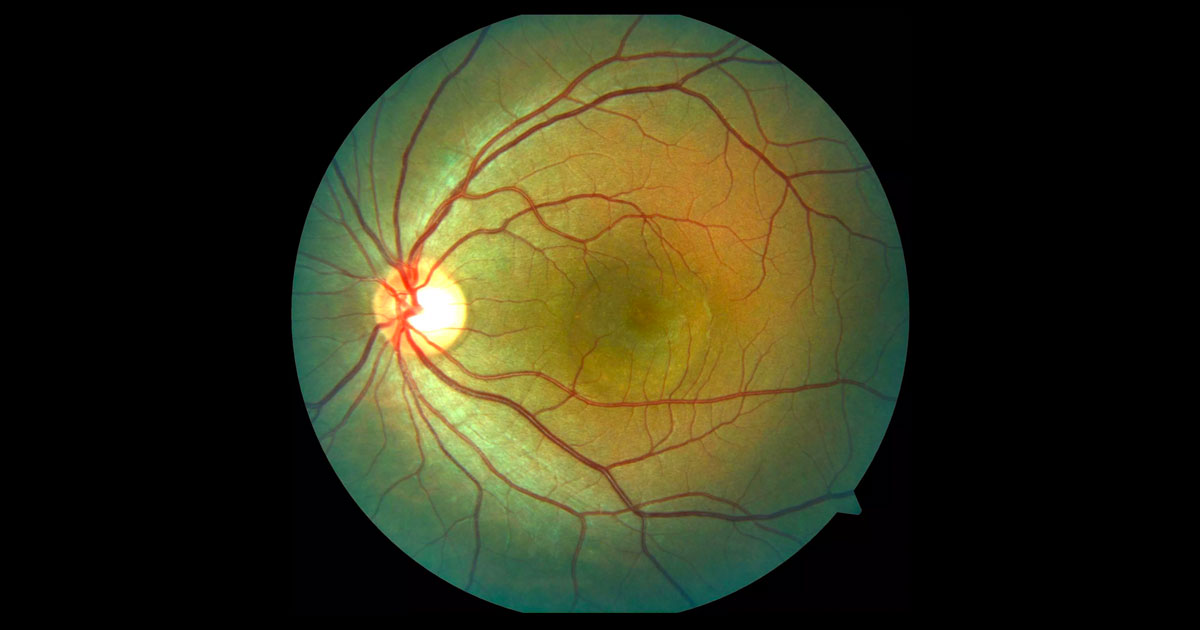
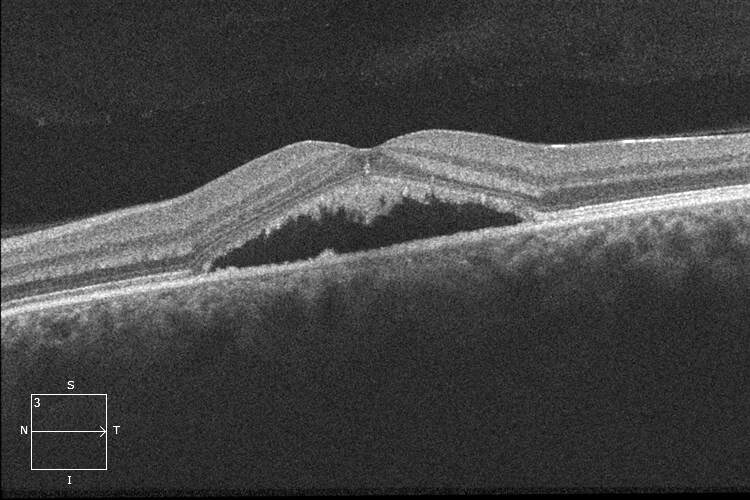
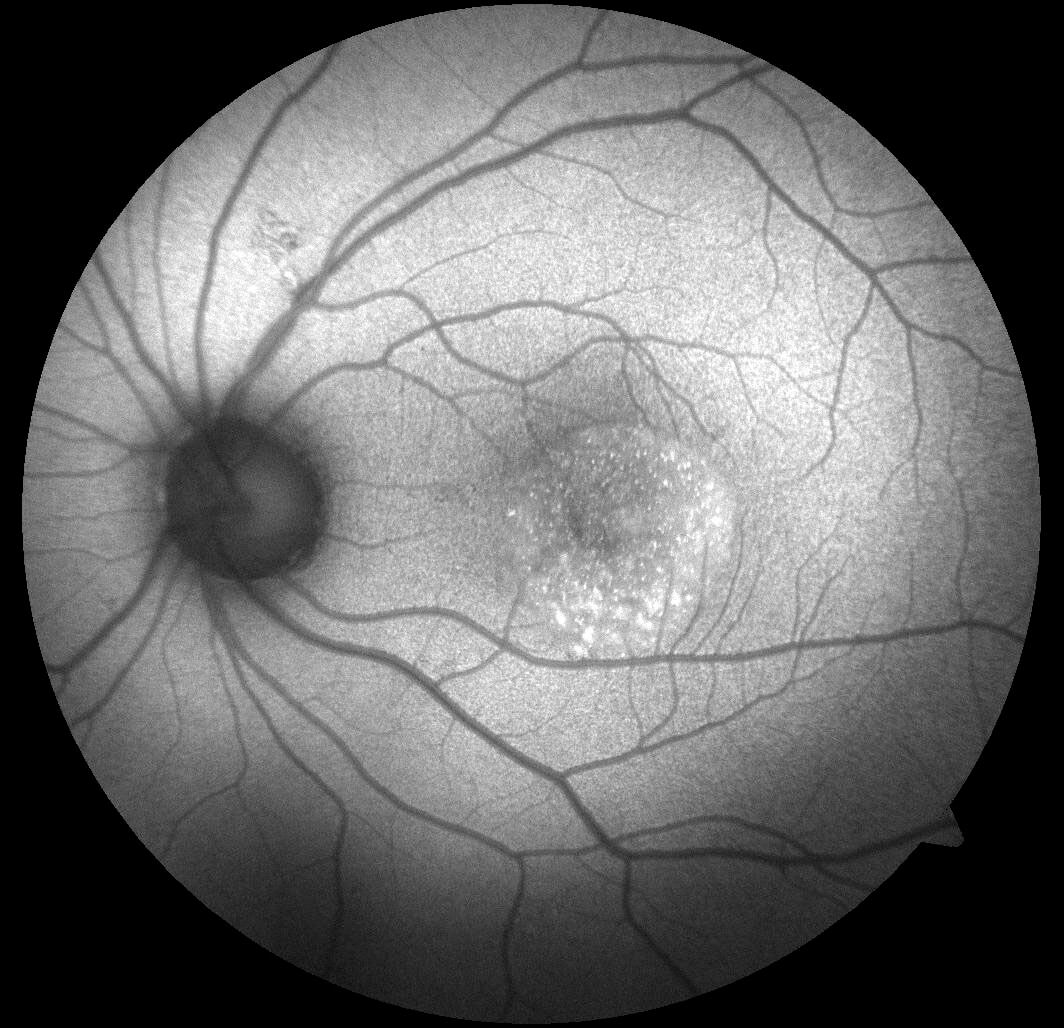
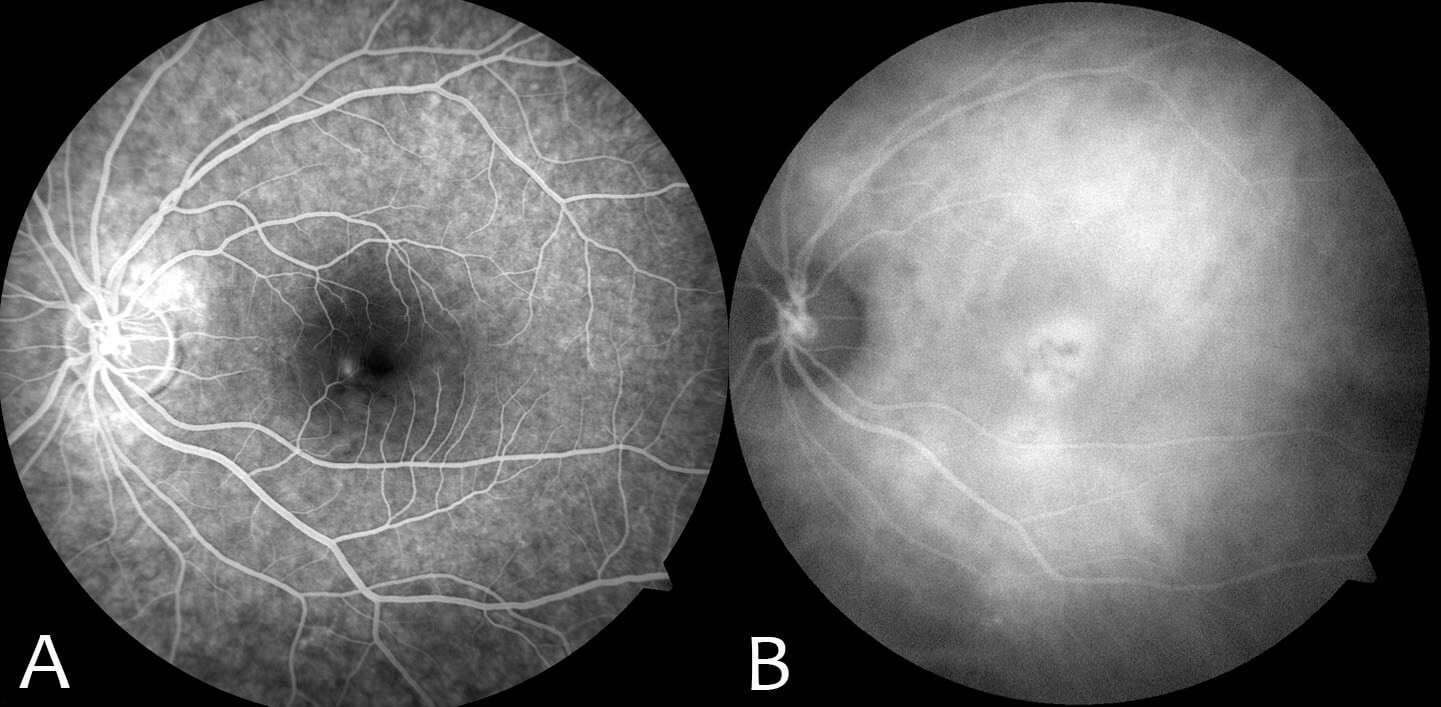
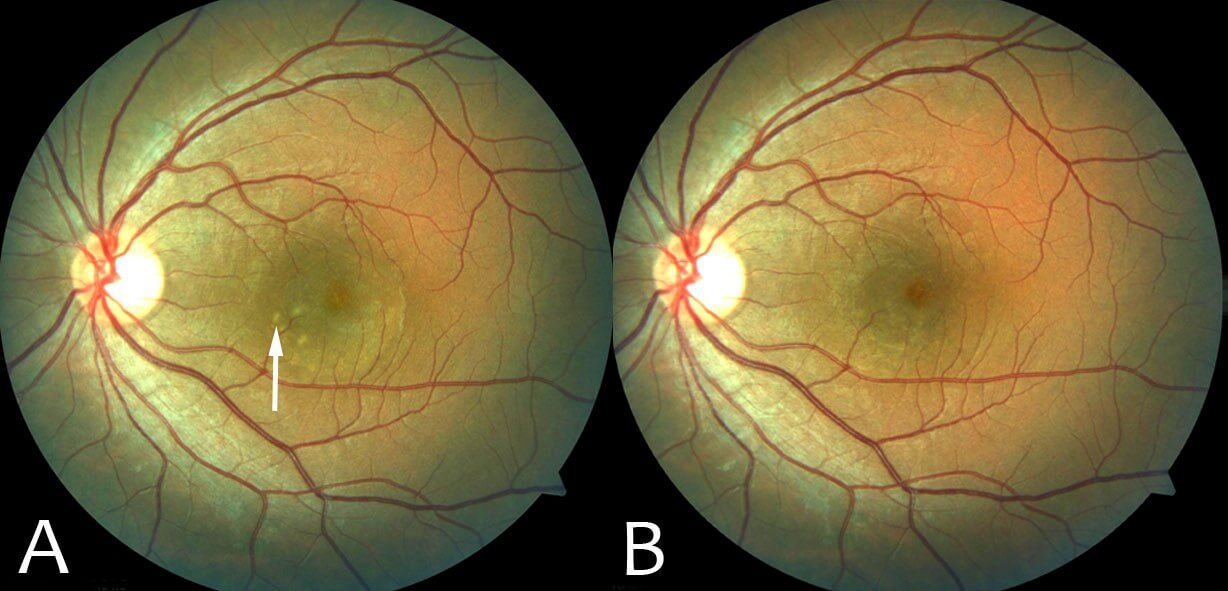
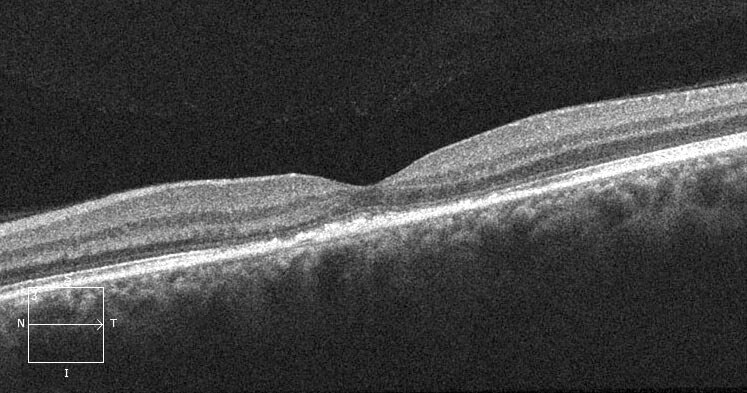
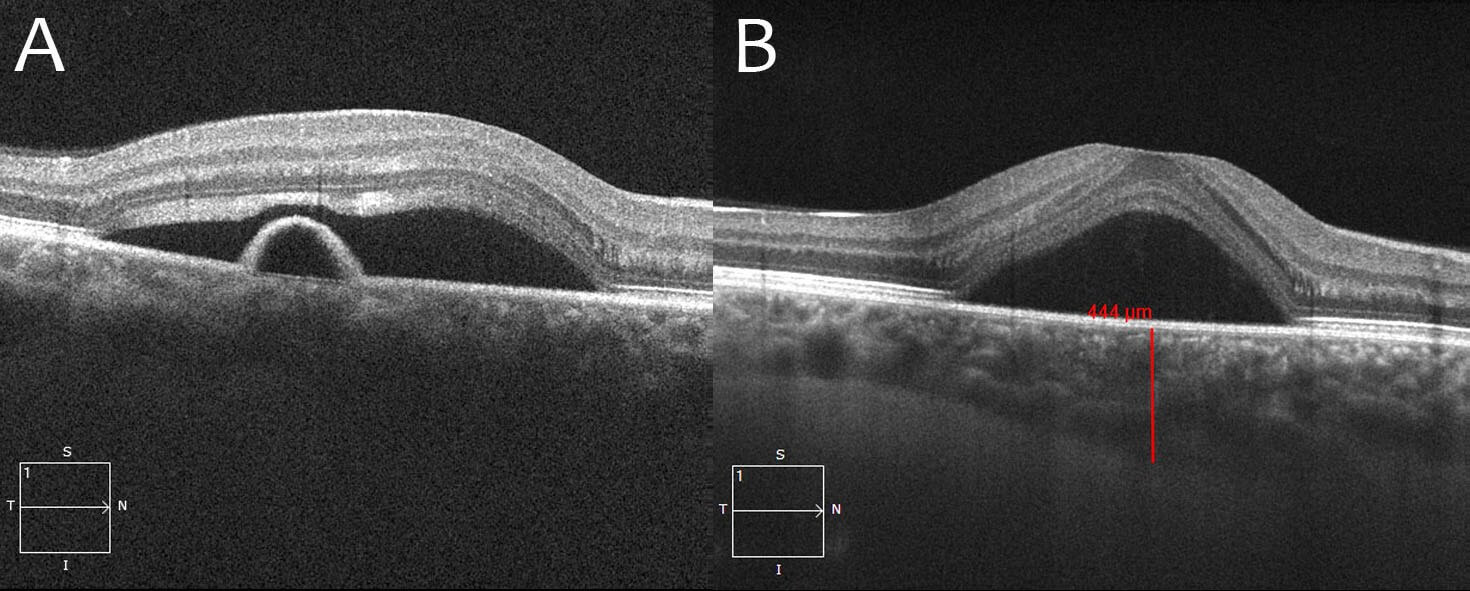
Red flags in the diagnosis of CSC include:
- Age over 50 years (need to consider neovascular AMD).
- Female patient unless pregnant (CSC is 6-8 times more common in men).(4)
- Presence of macular haemorrhage (consider CNV or polyps). However, in some cases CSC may be complicated by CNV.(6)
- Pathological myopia. While CSC can occur in myopia(7) it is more common in hypermetropes. In high myopes, myopic CNV or a dome shape macula configuration need to be considered.
Most cases of CSC will resolve spontaneously within 3-4 months.
(8) There is however a high recurrence rate with almost 50% of patients having a further episode within the next year.
(9) The most important and easily reversible risk factor for the condition is corticosteroid usage (oral, topical, inhaled, nasal spray, intra-articular). Eyecare professionals should liase with the patient’s physician to stop or minimise the dose of the medication where it is safe to do so. Other described risk factors include type A personality, phosphodiesterase inhibitors (e.g. Cialis and Viagra), obstructive sleep apnea, hypertension and pregnancy.
(1) Since most cases resolve spontaneously within 4 months, modification of reversible risk factors and observation is the usual management.
(1)Persistent submacular fluid can cause irreversible macular damage.
(1) Accordingly most retinal specialists intervene if there has been no improvement following 3-6 months of observation. Fluorescein and indocyanine green (ICG) angiography is used to guide treatment. If angiography demonstrates focal leakage away from the foveal centre, argon laser can be used to promote subretinal fluid reabsorption. Although the precise mechanism is not known, it may seal focal RPE defects, promote the recruitment of nearby RPE cells or improve the pumping function of RPE cells.
(1)If there is no focal leakage, or it is too close to safely treat with argon laser, reduced fluence photodynamic therapy (PDT) has been reported to have a close to 95% success in resolving subretinal fluid.
(10,11) It has a good safety profile but risks include choroidal ischaemia and RPE damage, both of which can result in irreversible vision loss.
(1) An intravenous medication (Visudyne® (verteporfin)) is injected intravenously before being activated by the PDT laser. In Australia, verteporfin is only listed for treatment of neovascular AMD and an application for compassionate usage has to be made to the Therapeutic Goods Administration (TGA) and manufacturer for its supply in patients with CSC.