-
Retina and Macular Diseases
Age-related macular degeneration (AMD)
AMD is the most common cause of vision loss over 65 years. It can present as blurring and/or distortion of central vision. Two forms exist: The “dry” form where there is wearing of the macula, and the “wet” form where there is bleeding. The “wet” form can be treated by medicines given into the vitreous jelly of the eyeball.
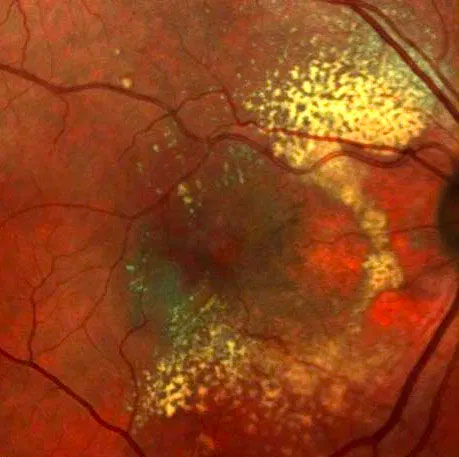
Diabetic retinopathy
Patients with diabetes can develop changes in their retina. Although these changes can result in blurring of vision, it can also go unnoticed until the disease is quite advanced. Complications of diabetic retinopathy can be serious, and include retinal detachment or bleeding. For this reason, all patients with diabetes should be checked regularly by an optometrist or ophthalmologist.
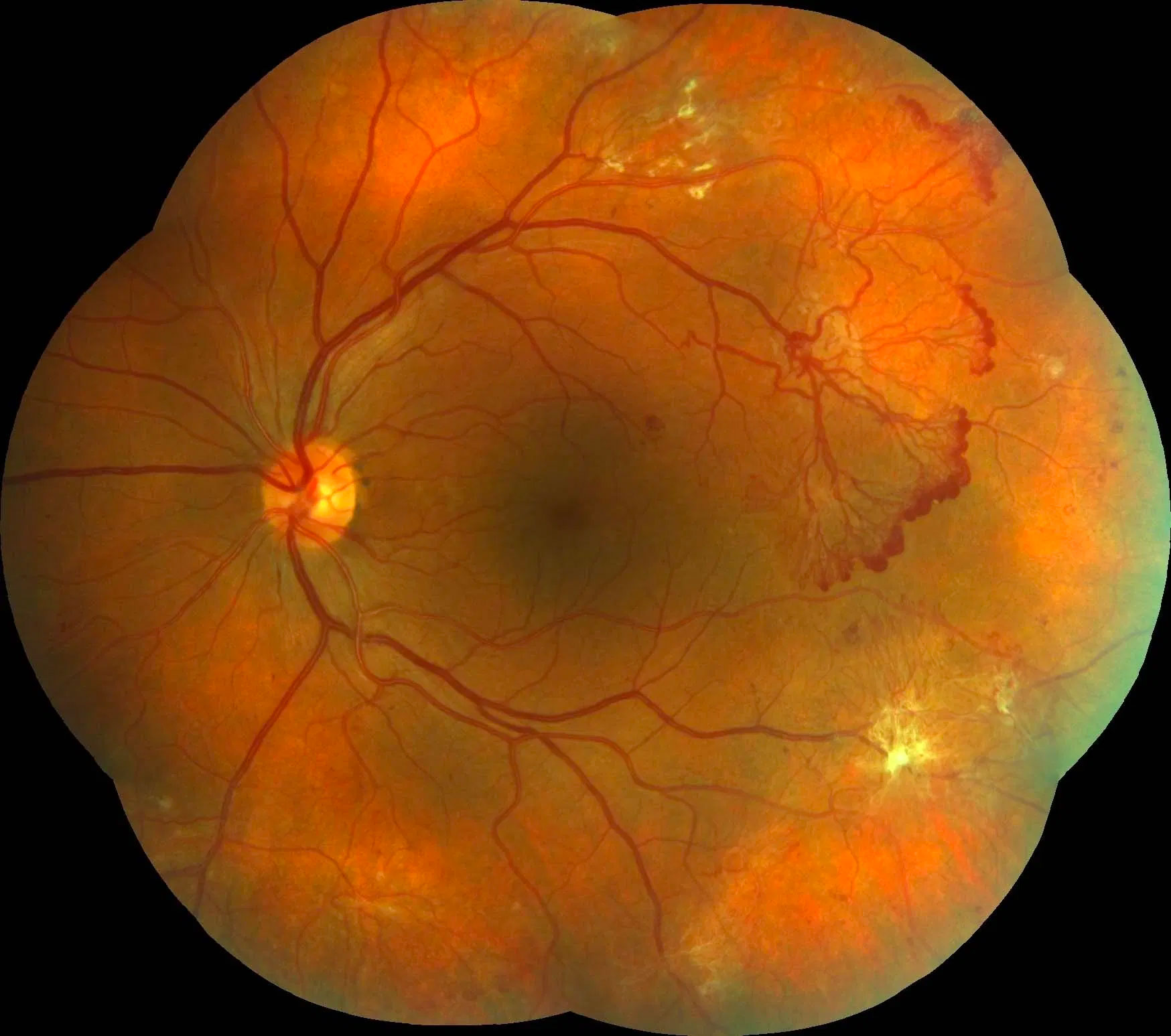
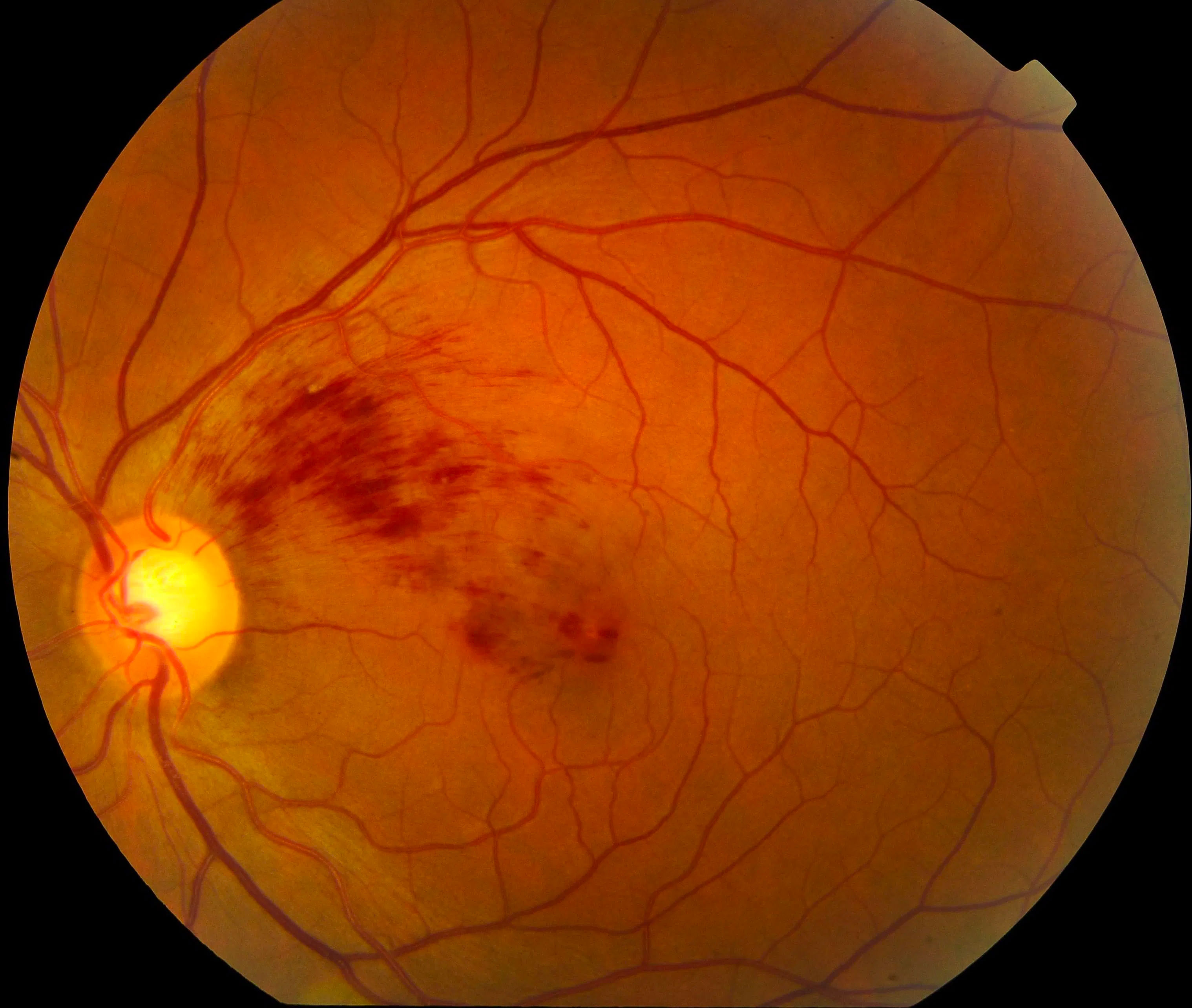
Retinal vascular occlusions
The retina has its own blood supply. If these vessels are blocked, it can lead to loss of vision. Retinal vascular occlusions can present as blurring and/or distortion of vision.
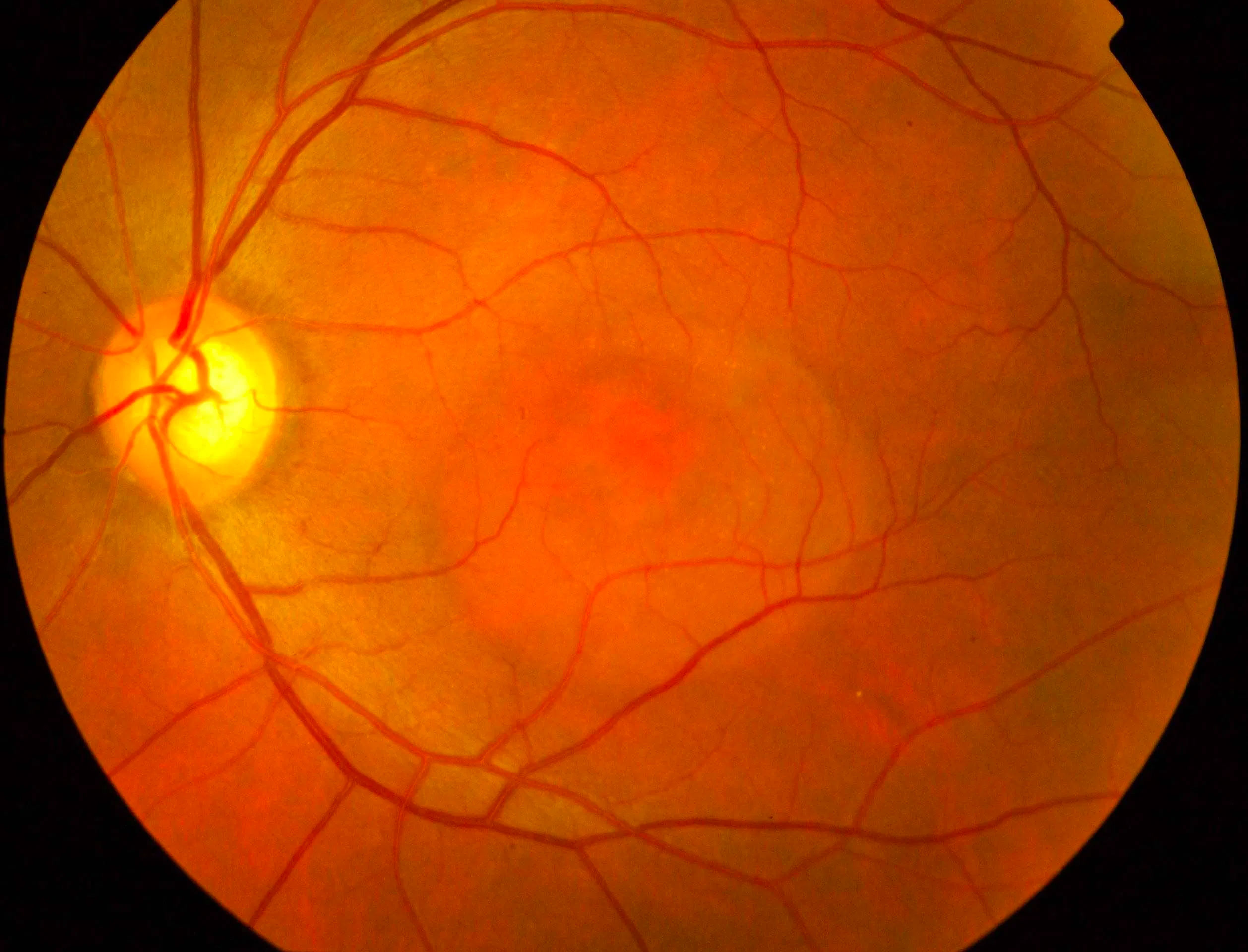
Central serous chorioretinopathy (CSC)
CSC is a condition where there is a build-up of fluid underneath the retina, often at the macula. It frequently occurs in young to middle aged males. Steroids are a risk factor. It can present with blurring and/or distortion of vision, and the sensation that images look smaller in the affected eye.
Pathological Myopia
Patients who are very short-sighted (myopic) have a high incidence of many retinal diseases, including: retinal tears and detachment, macula hole and choroidal neovascularisation.
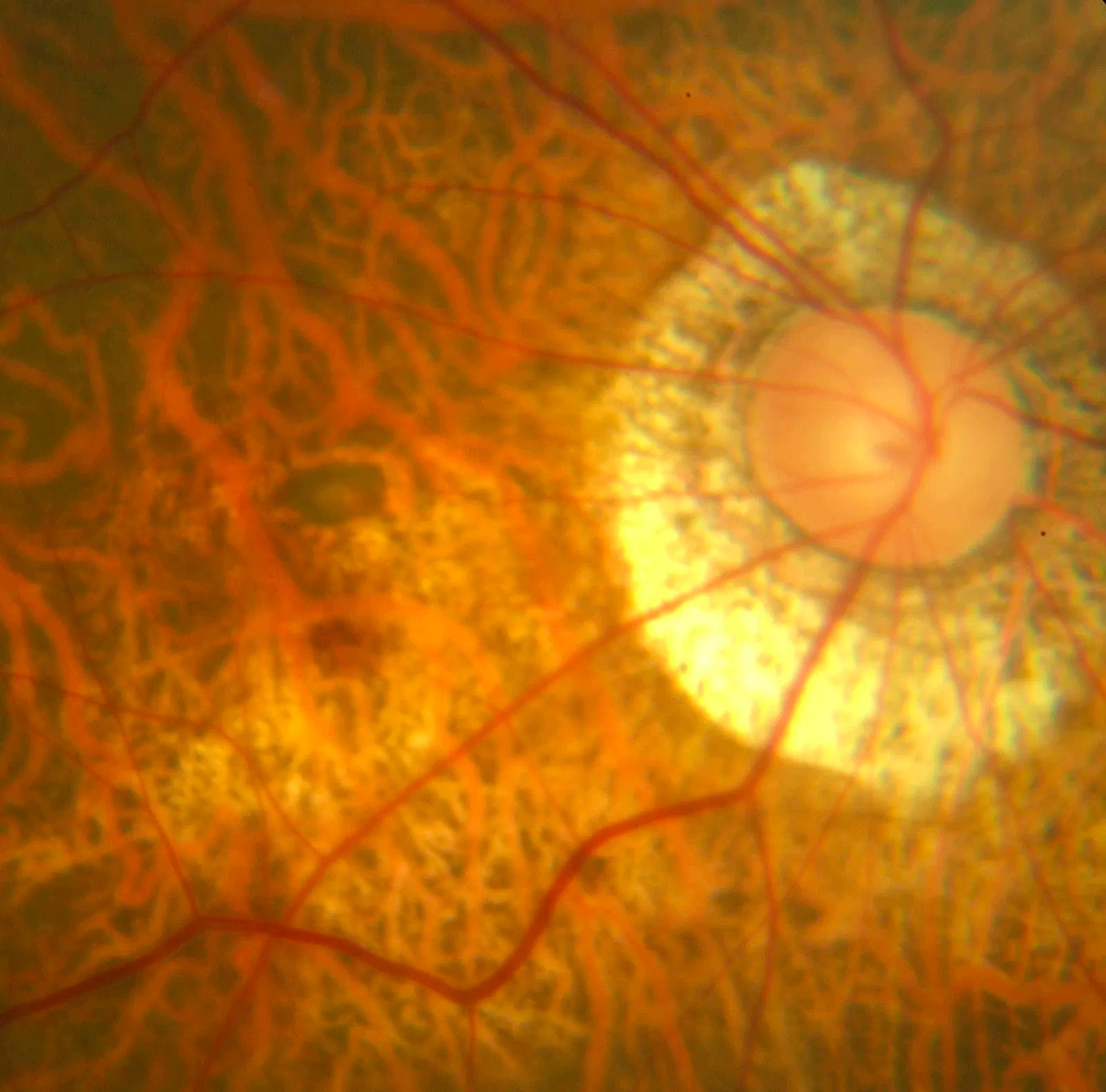
Retinal tears and detachment
Retinal tears can be associated with “flashes” and “floaters” or hazy vision. In addition to these symptoms, a retinal detachment can also cause blurring of peripheral vision (like a “curtain” or “shadow”), which untreated can progress to blurring of the entire vision. Any new onset of “flashes” or “floaters” or a “curtain” in the vision requires urgent examination by an ophthalmologist. Both retinal tears and detachment are normally painless Individuals who are very short-sighted or who have had cataract surgery are at an increased risk of retinal tears or detachments.
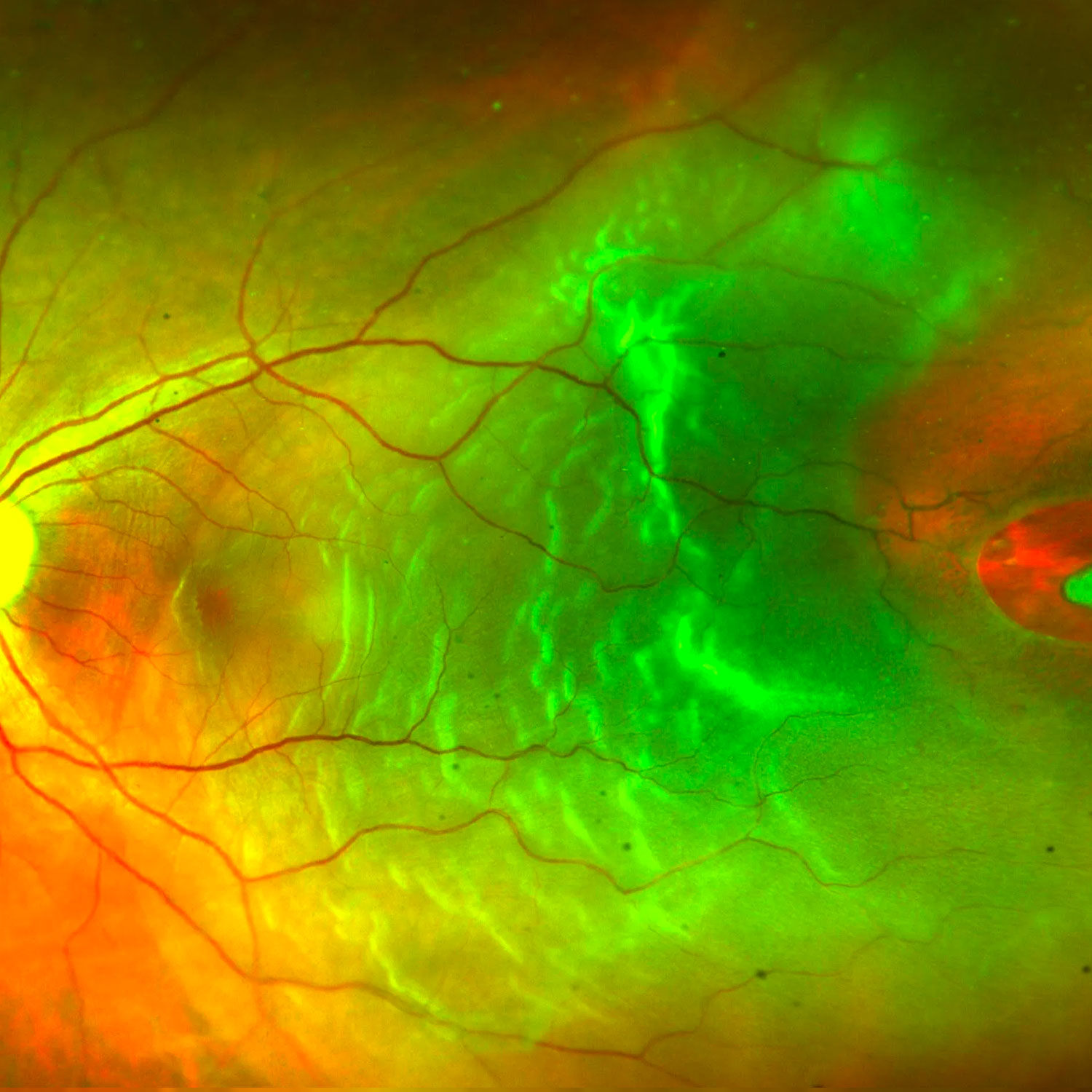
Vitreous haemorrhage (bleeding)
If there is bleeding in the vitreous this can cause the vision to be hazy. Common causes include a retinal tear or detachment, diabetes or a vascular occlusion.
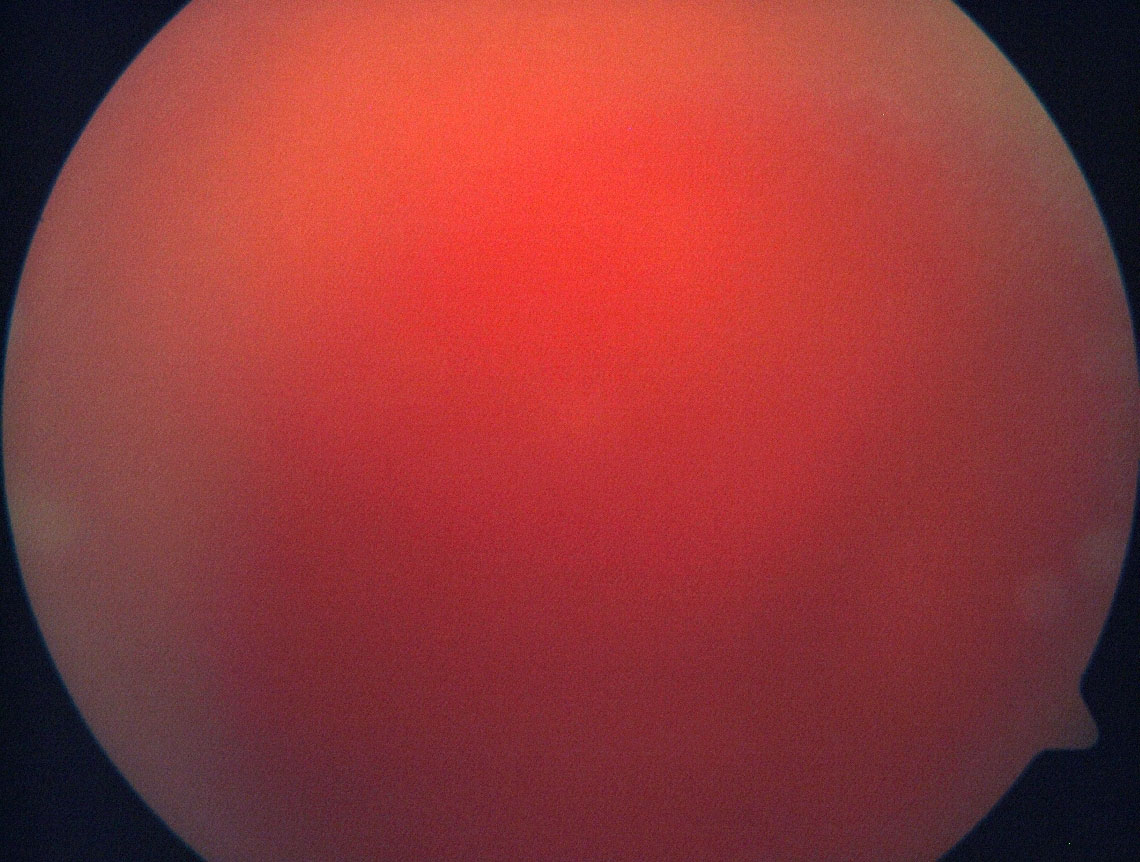
Epiretinal membrane
An epiretinal membrane is a scar tissue that lies on the surface of the retina. This can cause the retina to wrinkle or swell, resulting in blurring and/or distortion of central vision.
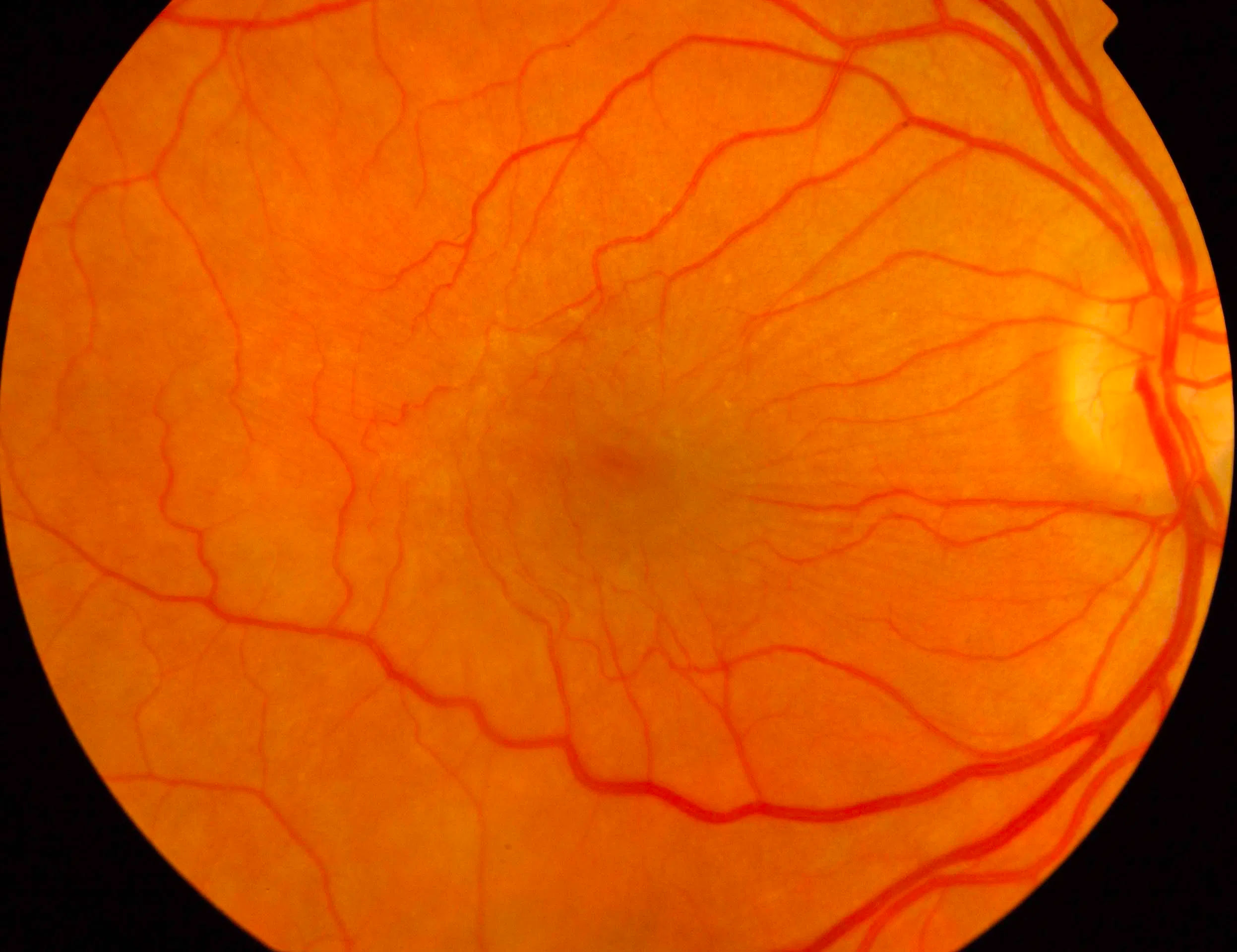
Macular Hole
A macular hole occurs when there is a defect in the retina at the macula. This can cause a black spot in the central vision, with blurring and distortion.
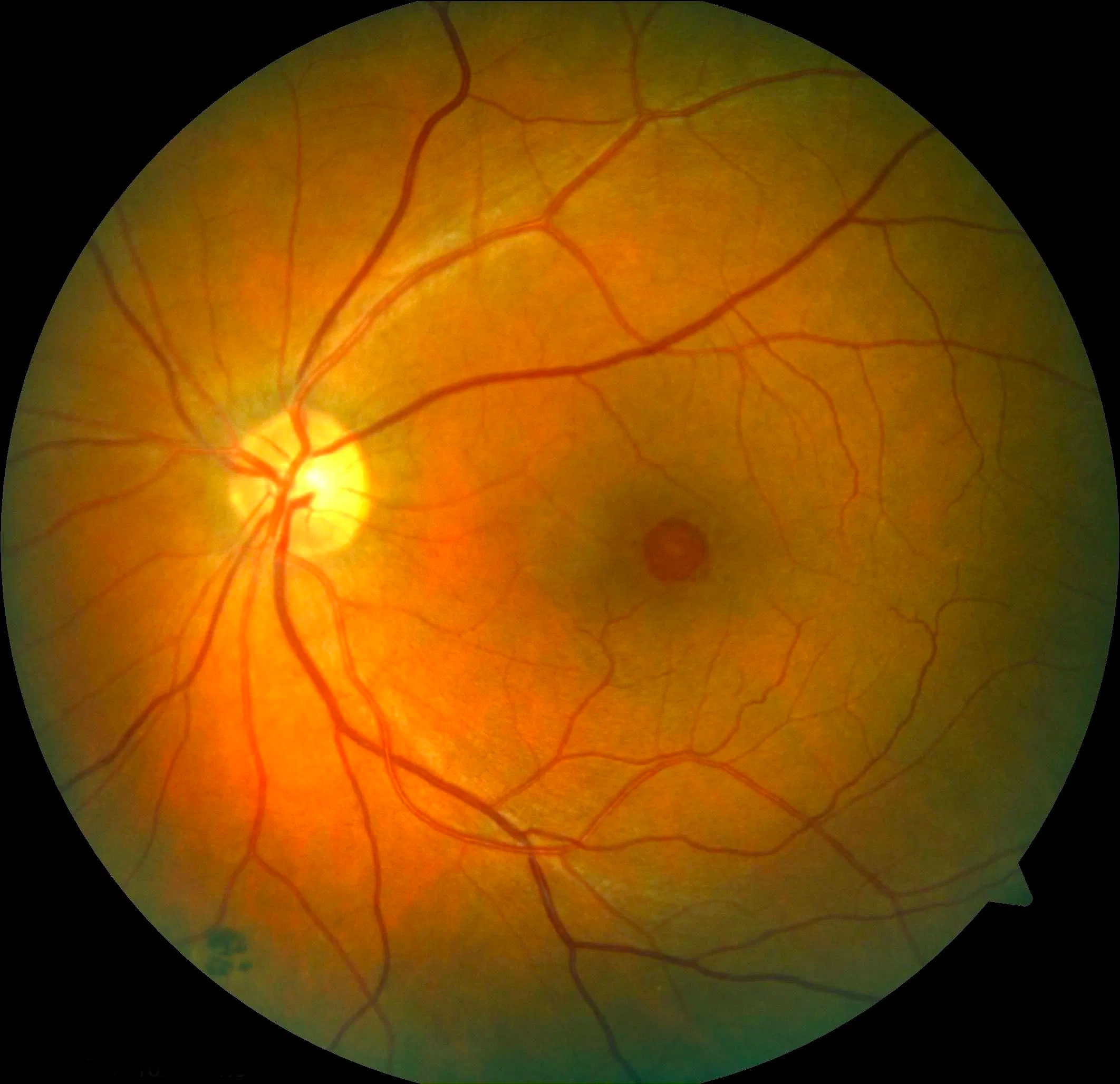
Eye inflammation
Many conditions can cause inflammation in the eye. Some of these are related to medical illnesses affecting the rest of the body, and some are caused by infections. Eye inflammation can cause redness, pain, sensitivity to light, “floaters” and blurring and/or distortion of vision.
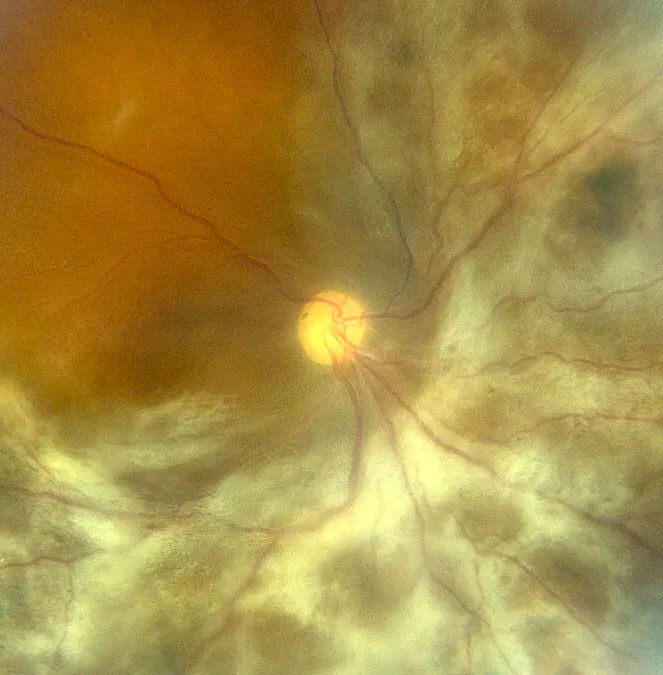
Eye tumours
The most common tumour originating from the eye is a naevus (“freckle”) within the choroid. Similar to freckles found on the skin, these spots in the eye need to be monitored as there is a small possibility of them developing into melanomas. Melanomas in the eye may not cause any symptoms. In other cases melanomas can cause “flashes” and blurring and/or distortion of vision.
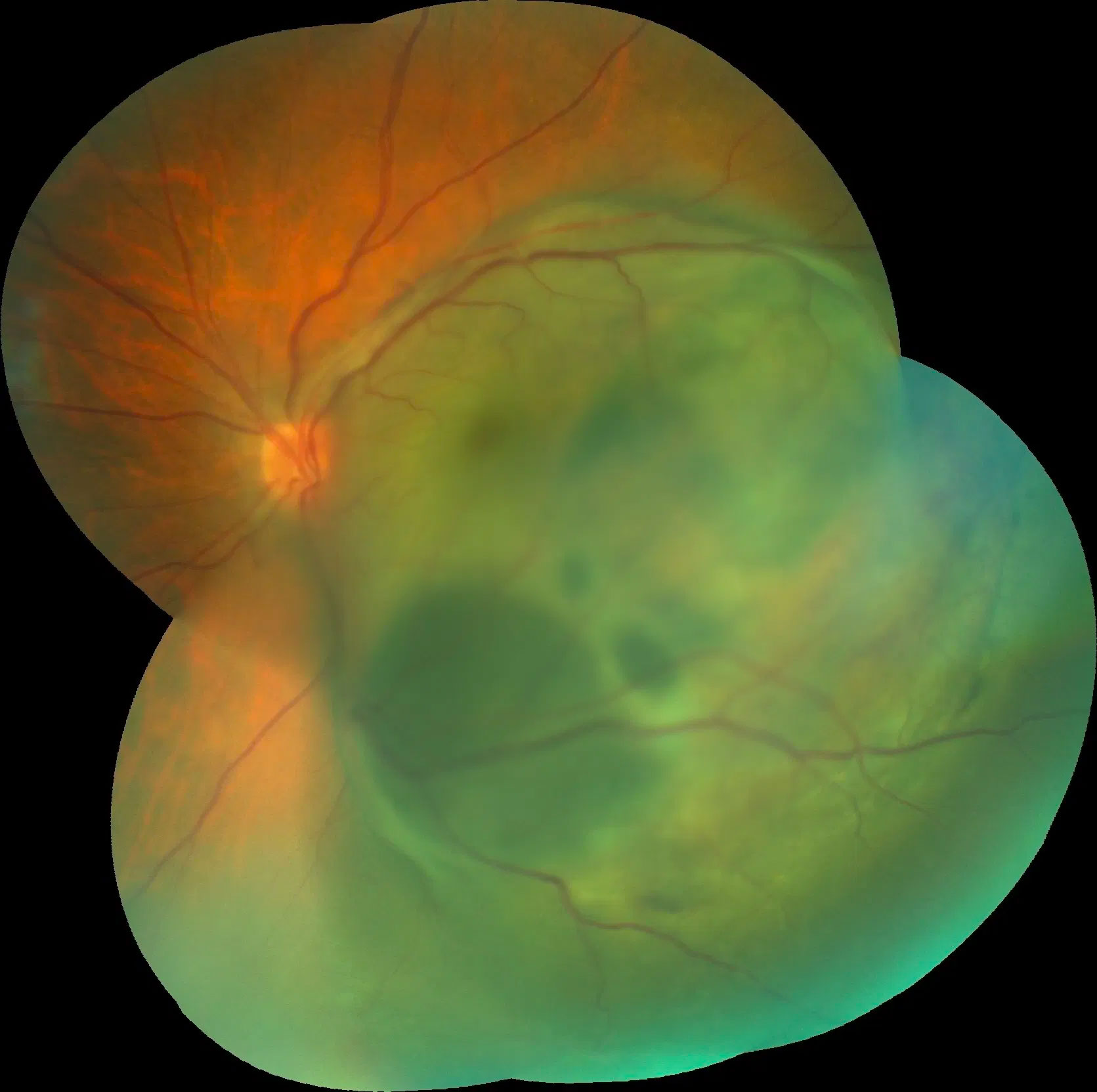
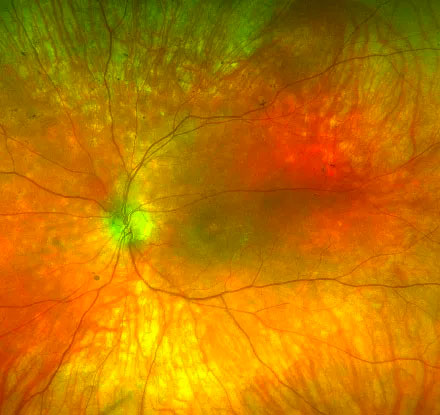
Inherited Retinal Diseases
Some retinal diseases have a genetic basis. There are often rare and include Retinitis Pigmentosa and Stargardt Disease. Symptoms vary depending on the disease but may include blurring and/or distortion of vision, colour vision impairment, poor peripheral vision and reduced night vision or slow dark adaptation. The optic nerve is the main cabling through which the eye transmits images to the brain for processing.
-
Cataracts
We all have a natural lens that sits behind the iris or coloured part of the eye. The function of the lens is to focus incoming light onto the back of the eye so that we can see. As we get older, the lens can slowly become cloudy. This is known as a cataract. Eventually, this can affect the ability of light to reach the back of the eye, resulting in symptoms such as blurred vision, glare, and difficulty with activities such as driving at night. Cataracts are more common in older people but can occur at any age.

A normal eye vs an eye with a cataract (white discolouration)
-
Glaucoma
Glaucoma refers to a group of eye conditions in which there is a progressive deterioration of a patient’s optic nerve. The optic nerve is the main cabling through which the eye transmits images to the brain for processing.
Glaucoma often doesn’t have symptoms in the early stages. It starts by affecting your side, or peripheral, vision which usually goes unnoticed until the nerve damage becomes so advanced that the central vision is affected. Unfortunately the optic nerve damage and vision loss that occurs in glaucoma cannot be reversed. For this reason, early detection and diagnosis of glaucoma is critical so that treatment can be started to prevent further vision loss.
Glaucoma diagnosis
As early glaucoma is largely asymptomatic patients need to have regular eye examinations to screen for the early signs of glaucoma. We encourage our patients to have regular eye examinations of their optic nerve, intraocular pressures and visual fields, which are the principle ways to detect glaucoma. This particularly applies to high-risk patients such as those who have a family history of glaucoma or those older than 65 years of age.
Our ophthalmologists have access to the latest diagnostic equipment for detecting glaucoma before it becomes advanced including:
- Heidelberg and Zeiss Spectral Domain Optical Coherence Tomography (OCT) to detect early signs of damage to the optic nerve.
- Zeiss Humphrey Field Analyser
Glaucoma treatment
The main way that glaucoma is treated is by lowering the pressure in the eye (intraocular pressure, IOP). This can slow or stop further damage to the optic nerve and thereby prevent further vision loss and blindness in most cases. As existing vision loss from glaucoma cannot be recovered, early detection and treatment is critical. Common ways to treat glaucoma include eye drops, laser and/or surgery. Our specialist ophthalmologists will provide you with the latest information about your treatment options and work with you formulate a clear treatment plan.
Have a question? Call one of our clinics today.
© 2019- Eye Specialists Centre | Privacy Policy | Disclaimer | Website design:
