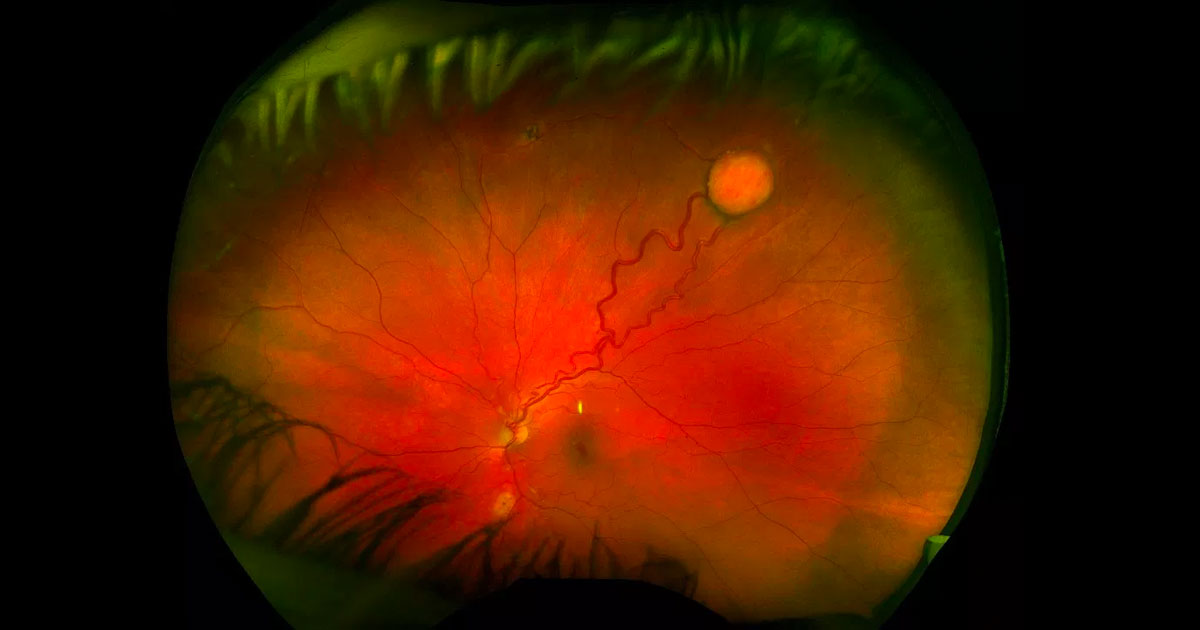
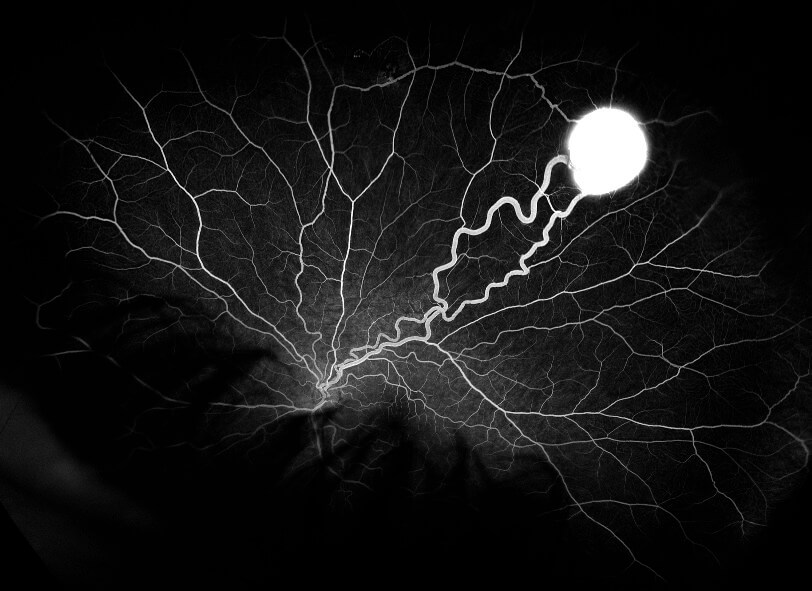
Retinal capillary haemangioblastomas (RCH) are circumscribed, orange-red vascular tumours of the retina with characteristic dilated feeding retinal arteriole and draining venule. They are most commonly located in the retinal periphery, especially superotemporally, although they can also occur at the optic disc (juxtapapillary RCH).(1) The mean age of diagnosis is 25 years in patients with von Hippel-Lindau disease but older (mean of 48 years) in patients with isolated disease.(2) One third of patients have multiple lesions and half have bilateral involvement.#references The differential diagnosis includes Coats Disease, vasoproliferative tumour, retinal arteriolar macroaneurysm, racemose hemangioma and retinal cavernous hemangioma. Fluorescein angiography is useful in assisting with diagnosis, confirming the vascular nature of these tumours.
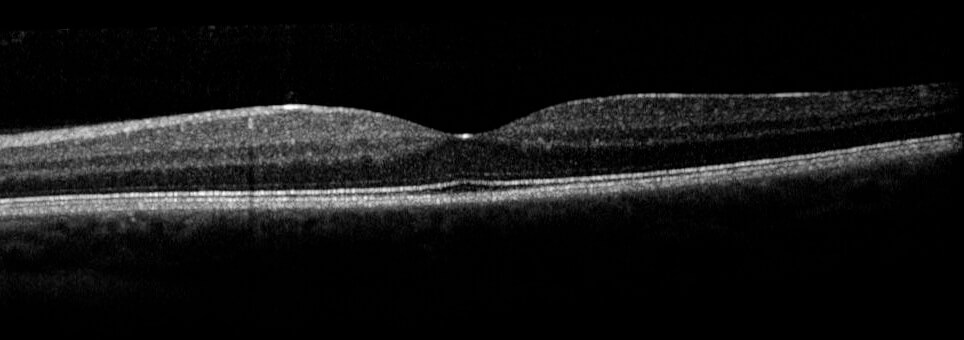
The most common complication is lipid exudation, which occurs in a quarter of cases.(1) This can start locally around the tumour but extend posteriorly causing a macular star with intra- and subretinal fluid affecting vision. Vision can also be affected by tractional retinal detachment. It is rare for retinal or vitreous haemorrhage to occur.
Retinal capillary haemangioblastomas can be isolated or associated with von Hippel-Lindau (VHL) disease. VHL is an autosomal dominantly inherited phakomatosis due to a mutation of the VHL gene on chromosome 3p25-26. The most common manifestation of VHL is RCH, which occurs in 49-85% of patients.(1) Conversely, the presence of an isolated RCH predicts VHL to be 30-46%.(3) Extraocular involvement in VHL can include haemangiomas of the central nervous system (brain especially cerebellum and spinal cord), cysts of the kidneys, adrenal glands, pancreas, inner ear, epididymis and broad ligament and tumours of the kidneys, adrenal glands (phaeochromocytoma) and pancreas. Diagnosis of VHL can be made by presence of:
- Greater than one RCH
- RCH with other systemic manifestations of VHL
- RCH with a family history of VHL
The diagnosis can be confirmed with genetic testing.
Small, isolated RCHs which are not associated with exudation or threatening vision can be monitored closely. Larger lesions and lesions associated with VHL are best treated, since they have a propensity to grow and affect vision via lipid exudation. The most common options for treatment include argon laser photocoagulation for more posterior tumours and cryotherapy for large anterior tumours associated with subretinal fluid. If laser is considered, treatment of the feeder vessel first before obliterating the tumour itself and/or draining venule may reduce the chance of haemorrhage. Often more than one session of laser or cryotherapy is required. Photodynamic therapy may be considered, especially for juxtapapillary tumours affecting vision. Severe cases associated with tractional retinal detachment may require vitrectomy surgery.