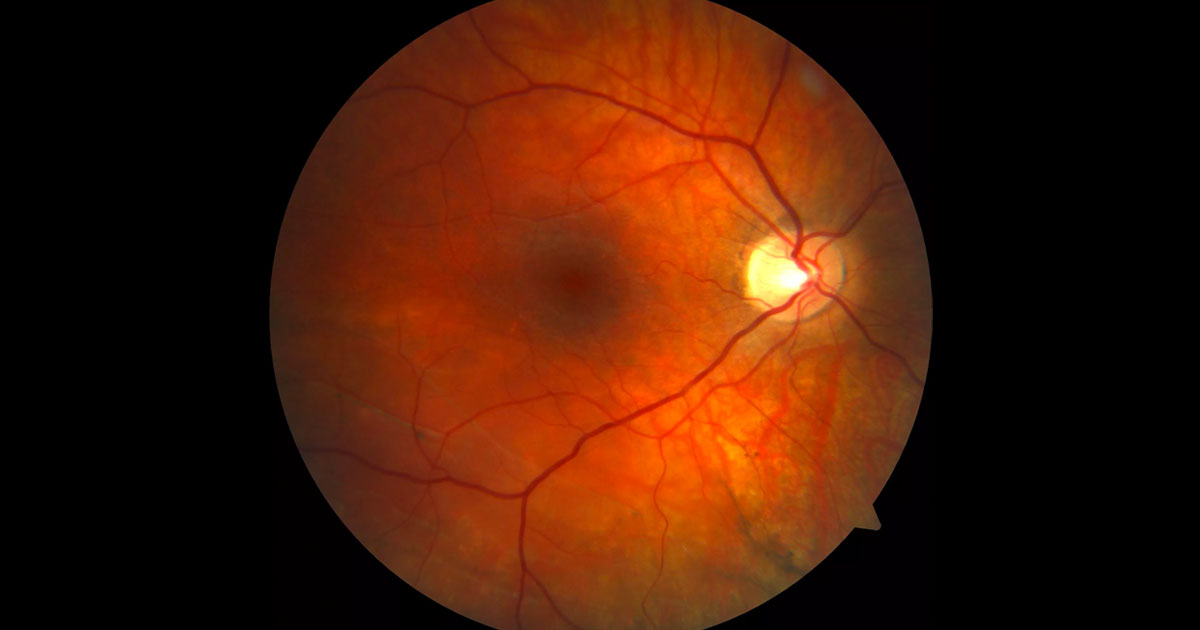
Figure 1. Colour fundus photography of the right macula. Prominent choroidal vessels suggests myopia. There is subtle subretinal elevation inferior to the fovea and horizontal white pigmented lines inferotemporally.
A 28-year-old male was referred with incidental retinal findings in his right eye.
A 28-year-old high myope was referred with incidental retinal findings in his right eye found on routine examination. He was asymptomatic and denied blurred vision, floaters, photopsia or a peripheral scotoma. He was a contact lens wearer correcting myopia of -7.5D in both eyes. He had no history of previous ocular trauma, surgery or laser. His optometrist noted the retinal changes in the right eye and referred him for a further opinion and management.
On examination his visual acuity was 6/6 bilaterally and intraocular pressures were normal. Anterior segment examination was unremarkable. Posterior segment examination demonstrated a tessellated fundus appearance in both eyes consistent with the high myopia. There was a subtle subretinal elevation inferior to the fovea and horizontal white pigmented lines inferotemporally (Figure 1).
DIAGNOSIS
Right asymptomatic chronic macula-splitting retinal detachment with “high water marks” (subretinal demarcation lines).
Further peripheral retinal examination demonstrated a right inferotemporal retinal detachment. The findings of inferotemporal atrophic holes within areas of lattice degeneration confirmed its rhegmatogenous nature. Additional atrophic holes with limited cuffs of subretinal fluid were noted superiorly. Lattice degeneration with associated atrophic holes were present inferiorly in the left eye.
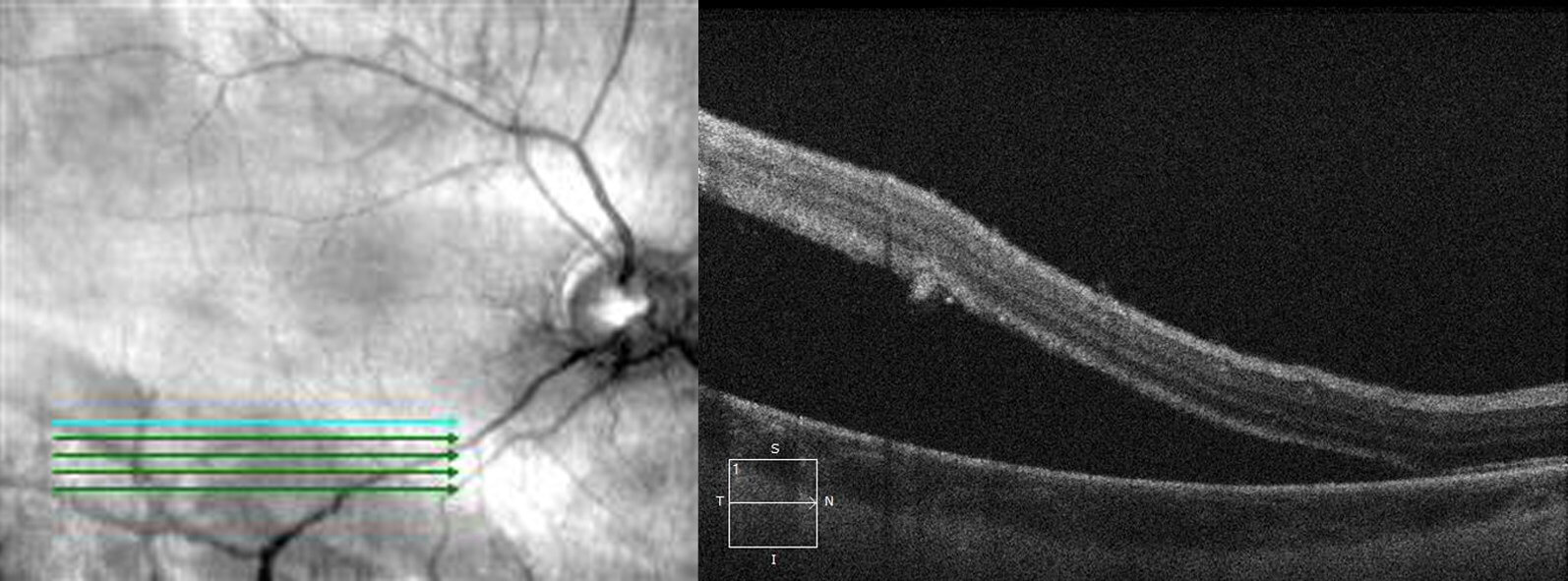
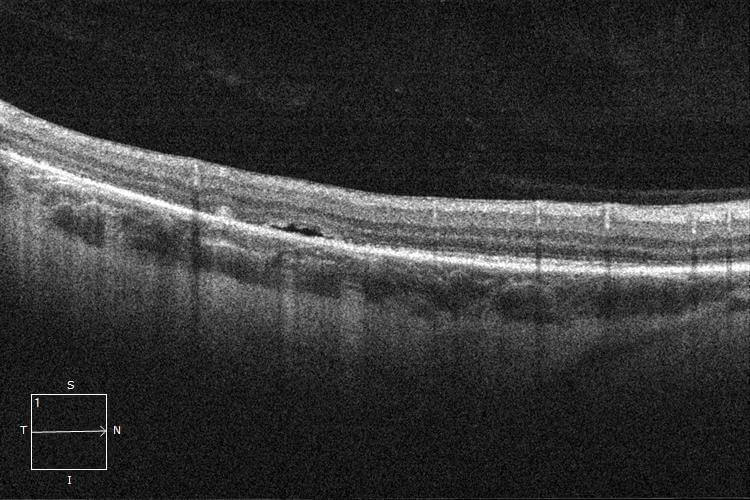
Optical coherence tomography (OCT) demonstrated extension of the retinal detachment within the inferior arcade but not involving the fovea (Figures 2 and 3).
Figure 2. Optical coherence tomography through the inferior right posterior pole demonstrates the retinal detachment.
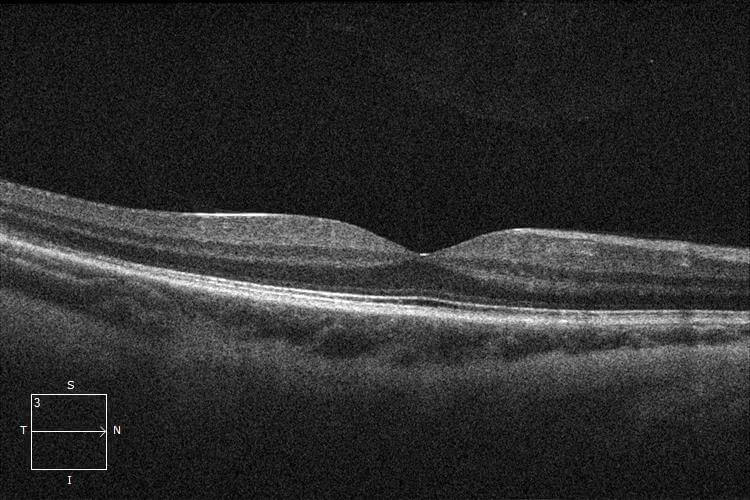
Figure 3. Optical coherence tomography through the right macula demonstrates foveal attachment (“macula-on”).
The findings were discussed with the patient. The patient was made aware of the risk of further progression to a macula-off retinal detachment and, particularly given its proximity to the fovea, was advised to have retinal detachment surgery.
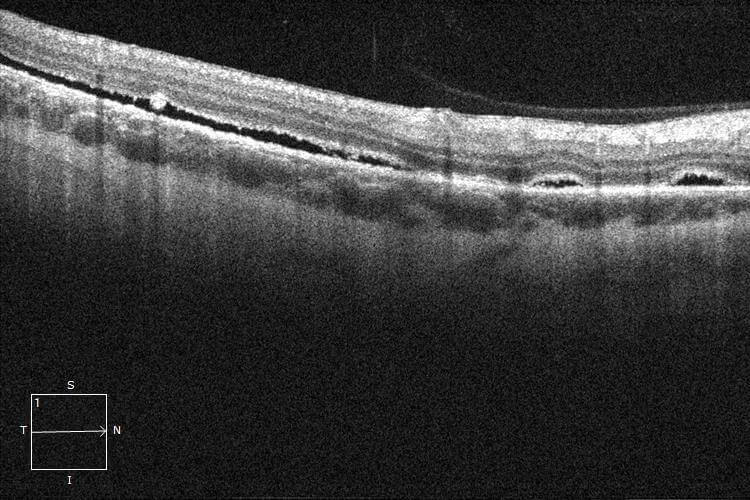
Scleral buckle surgery was performed including external drainage of the subretinal fluid. The patient remained relatively comfortable in the postoperative period and had an uncomplicated recovery with the retina successfully attached. Post-operative OCT imaging demonstrated minimal residual subretinal fluid which resolved after 6 months (Figure 4 and 5). The patient’s best corrected visual acuity remained 6/6 with a 1.0 dioptre myopic shift in his refraction.
The lattice degeneration and atrophic holes noted in the fellow eye was treated with prophylactic laser retinopexy.
Figure 4. One month post-operative optical coherence tomography demonstrated mild residual subretinal fluid. Note the areas of confluent fluid (left) and discrete blebs of subretinal fluid (right).
Figure 5. Six-month post-operative optical coherence tomography demonstrates almost complete resolution of the subretinal fluid.
Asymptomatic retinal detachments are occasionally noted as incidental clinical findings on routine examination. Typically, these are limited detachments in the far retinal peripheries which become symptomatic only when there is progression towards the macula. Atypically, our patient remained asymptomatic despite the retinal detachment extending to within the inferior arcade. Patients with asymptomatic retinal detachments will often be young myopes or have a history of blunt ocular trauma.
The demarcation or ‘high water marks’ noted in this case are often seen with chronic retinal detachments. They are caused by proliferation of RPE cells at the margin of the detached retina. They reflect the locations at which a retinal detachment has arrested at some stage.
In general, treatment options for retinal detachments include pars plana vitrectomy, scleral buckling, pneumatic retinopexy or occasionally barrier laser photocoagulation.(1) In asymptomatic retinal detachments few surgeons advise observation as the natural history is that they are likely to progress to symptomatic detachments at some stage in the patient’s lifetime.(2) In less-extensive, well-defined detachments that do not extend towards the arcades, barrier laser photocoagulation is a reasonable choice.(3) In young, phakic, myopic patients scleral buckling is often the preferred approach. This has the distinct advantages of avoiding post-operative cataract and also provides 360 degree support to the vitreous base. A disadvantage of scleral buckles however is that they frequently induce a myopic shift. Other complications specific to scleral buckles include diplopia and extrusion.
Small volumes of subclinical postoperative residual subretinal fluid are not uncommon after scleral buckling surgery. This may be seen on OCT imaging as areas of confluent fluid or discrete blebs of subretinal fluid which may take up to 12 months to resolve. If it involves the central macula this may delay visual recovery.(4)
Typically patients with lattice degeneration with or without round holes are at a very low risk for progression to clinical retinal detachment. It is reasonable however to prophylactically treat these areas in patients with rhegmatogenous retinal detachment in the fellow eye.
TAKE HOME POINTS
- Asymptomatic chronic retinal detachments are an occasional incidental finding on routine examination.
- Demarcation lines (“high water marks”) reflect the locations at which a retinal detachment has arrested at some stage.
- Scleral buckle surgery is often the preferred approach in young, phakic, myopic patients and particularly for inferior detachments.
- Subclinical postoperative residual subretinal fluid is common and can take months to resolve.
REFERENCES
- Schwartz SG, Flynn HW Jr, Mieler WF. Update on retinal detachment surgery. Curr Opin Ophthalmol. 2013; 24:255-61.
- Ahmad M and West J. Current opinion on treatment of asymptomatic retinal detachments. Eye 2007; 21: 1179–1185.
- Greenberg PB and Baumal CR. Laser therapy for rhegmatogenous retinal detachment. Curr Opin Ophthalmol 2001; 12:171-174.
- Benson SE, Schlottmann PG, Bunce C, et al. Optical Coherence Tomography Analysis of the Macula after Scleral Buckle Surgery for Retinal Detachment. Ophthalmology 2007; 114: 108-112.
Tags: myopia, retinal detachment