Toxoplasma gondii is an obligate, intracellular parasitic protozoan. Infection with this organism is the most common cause of posterior uveitis in non-immunocompromised individuals.(1) Sexual reproduction of the parasite occurs in small intestinal epithelial cells of the cat, with subsequent faecal elimination of oocysts. Once ingested by other animals, which serve as intermediate hosts, the oocysts rupture to release tachyzoites, which ultimately travel to target tissues to become tissue cysts or bradyzoites. Traditionally, it was thought that most active ocular toxoplasmosis represented reactivation of congenital toxoplasmosis acquired transplacentally from the mother. Recently, however, it has been shown that acquired infections occur more frequently than previously suspected.(2) Transmission can occur by ingesting oocysts, tachyzoites, tissue cysts or bradyzoites. In addition to contaminated food, water source contamination is increasingly recognized as a source of infection.
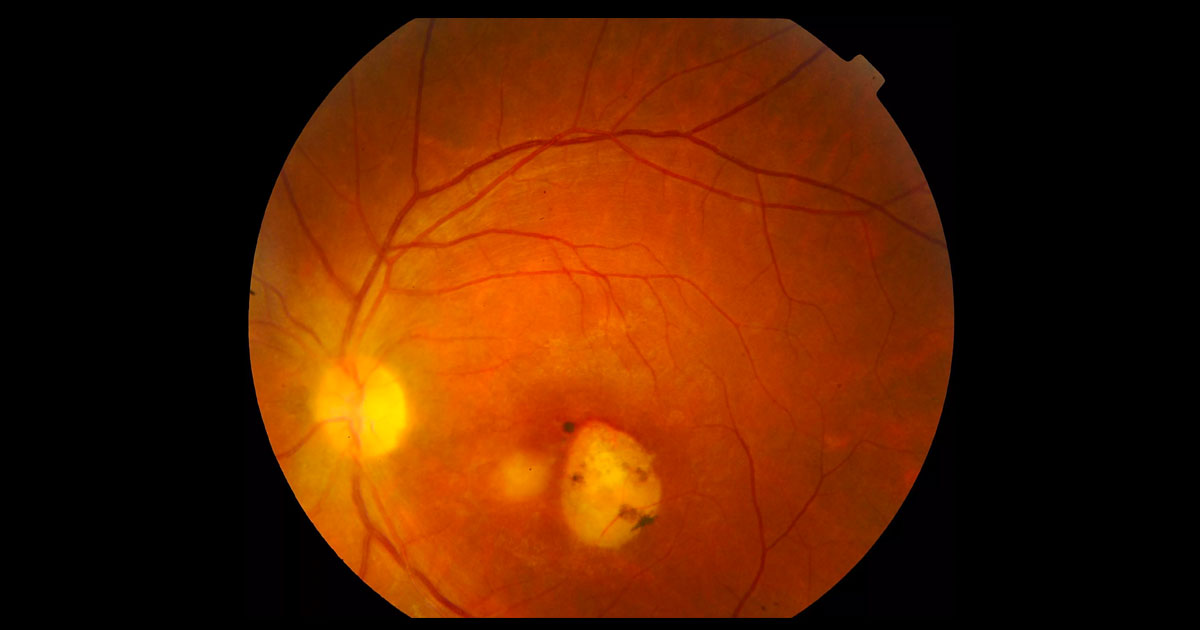
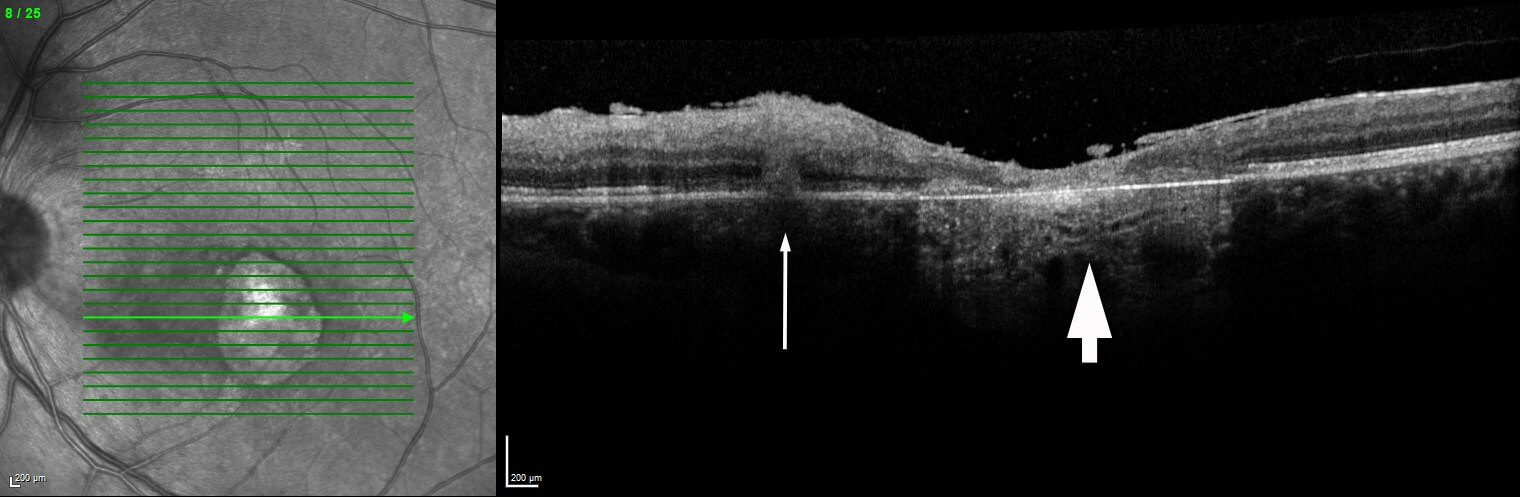
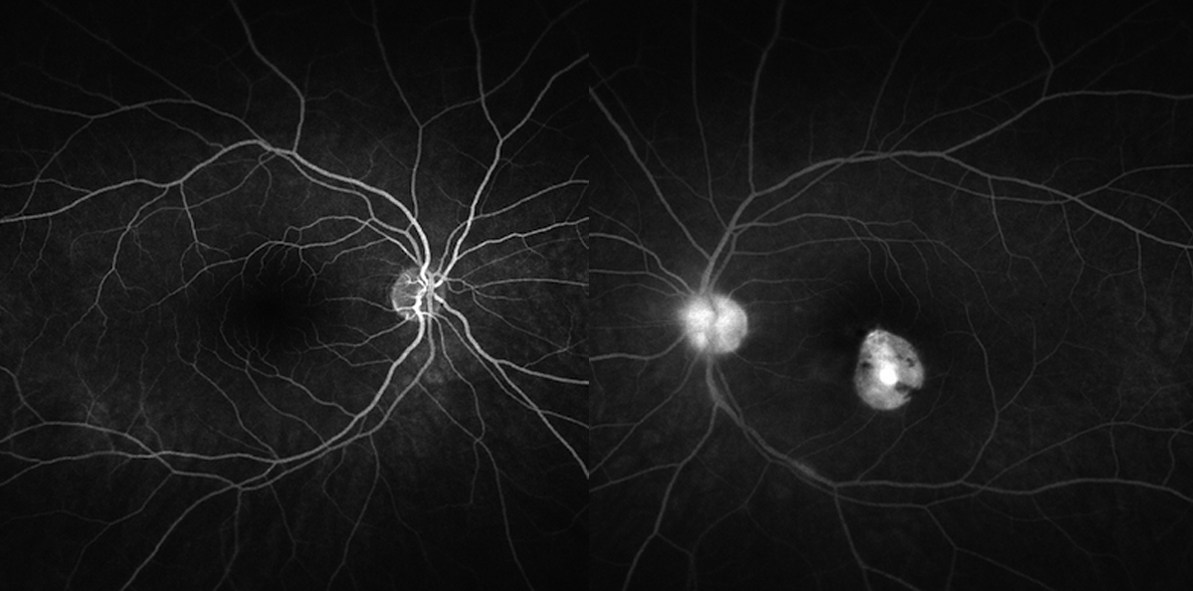
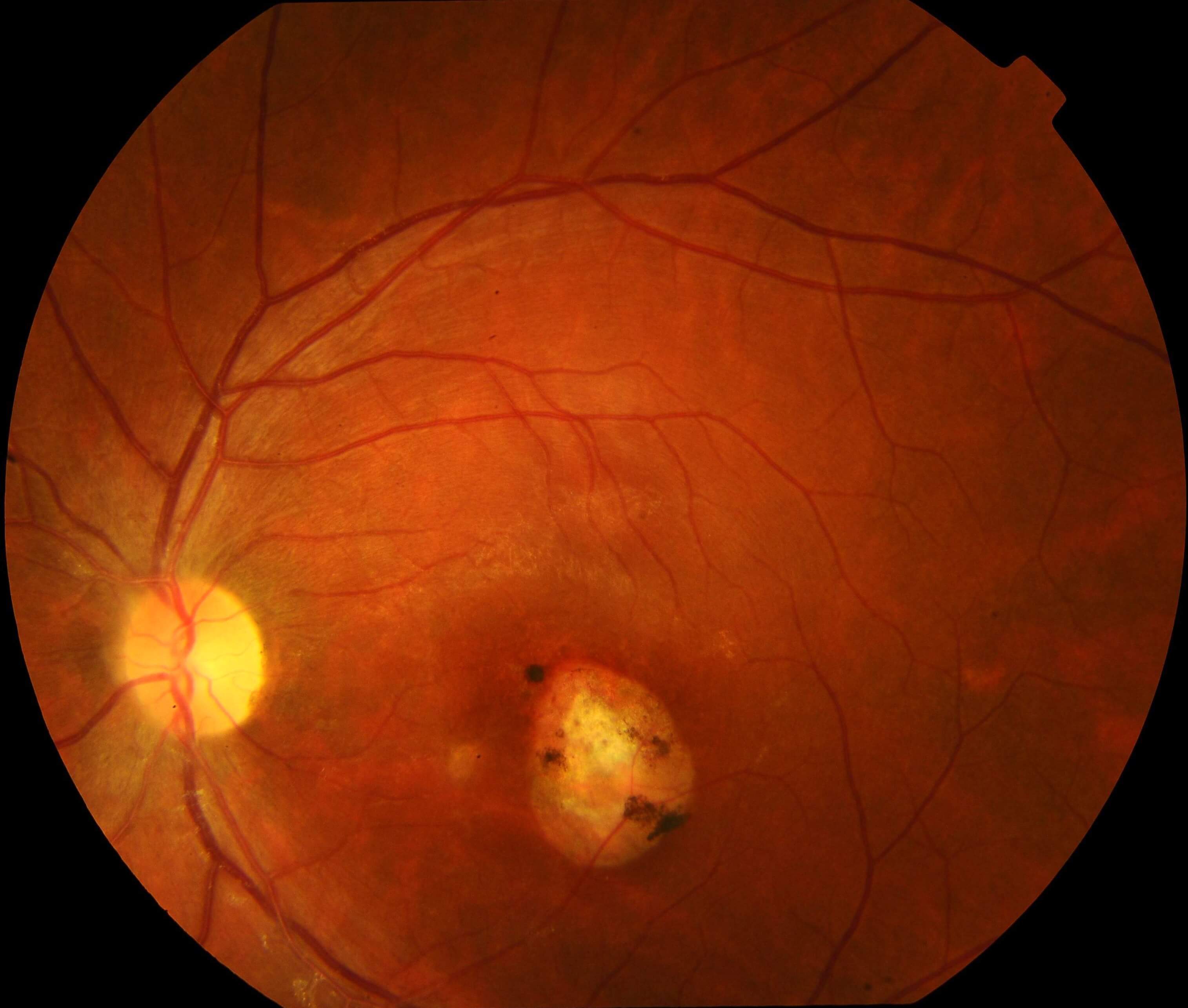
Toxoplasma infection is asymptomatic in most immunocompetent patients and, when it occurs, is usually benign and self-limited. The infection may be much more severe, however, in the foetus and immunocompromised patients. Ocular toxoplasmosis typically presents unilaterally as a focus of necrotizing chorioretinitis,(3) adjacent to a chorioretinal scar. There is usually a variable degree of intraocular inflammation involving the retina itself (oedema or localised retinal detachment), the retinal vessels (periphlebitis and/or segmental periarteritis), the optic nerve head (papillitis), the vitreous (vitritis, with precipitates on the detached posterior hyaloid), as well as the anterior segment (keratic precipitates, anterior uveitis, with or without elevated intraocular pressure).(3)
The diagnosis of ocular toxoplasmosis is made mainly by clinical observation of a focal necrotizing retinochoroiditis.(3) In atypical cases, serologic tests such as serum anti-Toxoplasma titres of IgM and IgG may be helpful to support the diagnosis. Negative IgG serology can help exclude ocular toxoplasmosis. Polymerase chain reaction of aqueous and vitreous samples has a high sensitivity and specificity.3
Non-sight-threatening lesions are frequently managed with observation. However, where the optic nerve, macula or a major retinal vessel are threatened or the vision is significantly restricted, therapy should be instituted.(4) Treatment includes prompt initiation of oral antibiotics as well as topical anti-inflammatory and cycloplegic agents. This is followed, usually 24-48 hours later, by the initiation of oral prednisone at high doses that are tapered slowly. Several antibiotics or combinations of antibiotics have been utilised with success.(5) More recently, treatment with an intravitreal combination of clindamycin and dexamethasone has also been shown to be successful.(6)
The recurrence rate of toxoplasmic retinochoroiditis correlates inversely with the period of follow-up, with a two year rate of up to 10 percent.(7) Long-term intermittent treatment with trimethoprim(160 mg)/sulfamethoxazole(800 mg) every three days may reduce the recurrence rate.(7)